Can I Get Social Security Disability Benefits for Ischemic Heart Disease?
- How Does the Social Security Administration Decide if I Qualify for Disability Benefits for Ischemic Heart Disease?
- About Ischemic Heart Disease and Disability
- Winning Social Security Disability Benefits for Ischemic Heart Disease by Meeting a Listing
- Residual Functional Capacity Assessment for Ischemic Heart Disease
- Getting Your Doctor’s Medical Opinion About What You Can Still Do
Residual Functional Capacity Assessment for Ischemic Heart Disease
What Is RFC?
If your ischemic heart disease is not severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process, the Social Security Administration will need to determine your residual functional capacity (RFC) to decide whether you are disabled at Step 4 and Step 5 of the Sequential Evaluation Process. RFC is a claimant’s ability to perform work-related activities. In other words, it is what you can still do despite your limitations. An RFC for physical impairments is expressed in terms of whether the Social Security Administration believes you can do heavy, medium, light, or sedentary work in spite of your impairments. The lower your RFC, the less the Social Security Administration believes you can do.
Adult ischemic heart disease that is significant but does not meet or equal the listing will require some type of residual functional capacity.
RFC Guidelines Regarding Exercise Test Performance
The Social Security Administration generally applies the following RFCs regarding exercise test performance:
- An abnormal test workload equivalent to an estimated 5 METs or less – Meets listing 4.04 part A if other criteria are satisfied. See Meeting Social Security Administration Listing 4.04A for Ischemic Heart Disease.
- A normal test workload equivalent exceeding 5 METs, but test positive at 6 METs or claimant unable to complete duration of 6 MET stage – sedentary work RFC.
- A normal test workload equivalent of 6 METs or more, but test positive at 7 METs or claimant unable to complete duration of 7 MET stage – light work RFC.
- A normal test workload equivalent of 7 METs or more, but test positive at 8 METs or claimant unable to complete duration of 8 MET stage – medium work RFC.
- A normal test workload equivalent of 8 METs or more, negative test for completing full 8 MET stage or more – heavy work or “not severe.”
Environmental Restrictions
Once the general RFC is determined, further downward modification of the RFC may be indicated on the basis of environmental restrictions.
Factors that increase the heart’s work can cause the onset of ischemia and symptoms like angina, shortness of breath (SOB) and fatigue to occur at earlier levels of exertion than would otherwise be the case. An increase in blood pressure will have that effect. Environmental extremes like very hot or cold environments will increase physiological stress that does not occur from exercise testing in a nice, cool hospital or doctor’s office. For instance, heat or cold alone will drive up heart rate and leave less cardiac reserve for exertion.
An individual who can do medium work at a comfortable room temperature could reasonably be expected to be capable of no more than light work in hot or cold environments. Even healthy people are compromised in their exertional capacity in hot or cold environments, and individuals with heart disease are even more fragile in this regard.
Psychological stress can have the same effect, because it also increases the heart rate even before exertion begins. While it is obvious that certain occupations, such as being a police officer, are generally associated with high psychological stress, this is a rather murky area because such stress depends not only on the environment but the individual’s reaction to that environment. For example, some attorneys find litigation in a courtroom extremely stressful while others feel hardly a twinge of anxiety or even feel exhilarated by the experience.
Environmental limitations are sometimes overlooked by adjudicators. For example, if avoidance of temperature extremes is not mentioned on the RFC form, then the disability examiner or vocational analyst citing jobs you can still do will not apply that limitation. The consequences are that you may be cited a job that you cannot perform. If you are cited a job in which environmental extremes are involved, the RFC should be lowered one level from what it would otherwise be based on stress test results.
Environmental limitations that result in the elimination of your ability to return to prior work, restriction of applicable other work, lowering of RFC, and elimination of the “Grid” all present the opportunity for allowance of claims that would otherwise be erroneously denied.
Medications
Environmental work capacity is not just influenced by physiological stress, but also by medications. For example, consider a claimant with ischemic heart disease who has had heart failure. He takes a number of medications, including diuretics, that are carefully adjusted. The diuretics accelerate urinary fluid loss. If this person is exposed to extreme heat causing a lot of sweating, he may go into fluid imbalance and end up in the hospital. It is not reasonable to think that he can reliably adjust his water intake under changing conditions, although this can be accomplished to some degree. And it’s not just water that has to be replaced. Electrolytes (sodium, potassium) are likely to be moved out of normal range with possible serious consequences such as cardiac arrhythmias, increased weakness, and impairment in thinking.
Drugs known as beta-blockers, frequently used to treat hypertension and ischemic heart disease, suppress the ability to increase heart rate. This drug effect can affect the body’s ability to respond to the increased stress of temperature extremes.
Silent Cardiac Ischemia
It is possible to have very severe cardiac ischemia caused by marked coronary obstructive lesions and yet have no chest pain, weakness, or any other symptoms, i.e., “silent ischemia.” The Social Security Administration recognizes that silent ischemia must be considered in disability determination.
Severe silent ischemia appearing in the early stages of an exercise test is ominous. Even if a claimant has no history of symptoms such as angina that would qualify under the listing, an RFC limitation would be appropriate.
Other claimants may have abnormal ischemic resting ECGs that appear during routine monitoring of the heart for other purposes—such as 24-hour monitoring for an arrhythmia with a Holter monitor. Or they may simply have an abnormal resting ECG for the presence of ischemic heart disease even though they have no angina or other cardiac symptoms. In these instances also, some degree of RFC limitation in proportion to the severity of the abnormality should be given even if there are no symptoms.
Environmental stressors, especially extreme heat or cold, can make silent ischemia worse and perhaps even provoke symptoms such as angina or life-threatening arrhythmias that otherwise might be absent.
Cardiac Arrhythmias
Arrhythmias are most often related to the presence of ischemic heart disease in the adult claimant population. If a life-threatening arrhythmia appears at a particular stage of exertion on a cardiac stress test, that test should be considered positive and a factor in limiting RFC to a level of exertion at which the threat does not appear. As in other manifestations of ischemic heart disease, adverse environmental conditions such as heart or cold can produce further limitations.
Cognitive Losses After Coronary Artery Bypass Grafting
Problem of Cognitive Decline After Surgery
A great danger of coronary artery bypass grafting (CABG) (see Figure 7 below) is brain damage resulting in stroke (cerebrovascular accident, CVA). Some of these strokes result from surgical cross-clamping of the arch of the aorta during the operation when small pieces of atherosclerotic fatty matter can come loose and be pumped to the brain, where it lodges in an artery and blocks blood flow to some part of the brain.
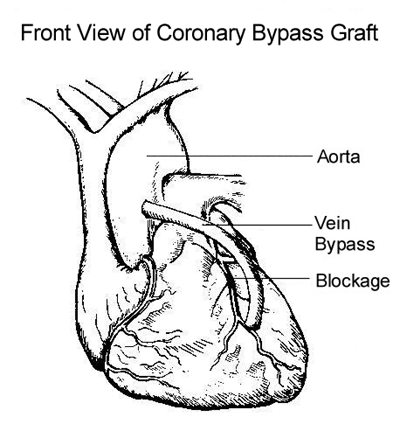
Figure 7: Revascularization via coronary artery bypass graft using a vein.
Even when no obvious stroke occurs, a person may have decreased reasoning ability (cognitive dysfunction) after CABG. While large strokes are likely to be obvious and included in the disability determination, significant cognitive dysfunction resulting from lesser degrees of brain damage, or brain damage to areas not involved in movement, can be missed.
Cognitive decline after CABG affects 16-42% of patients. The possibility of brain damage is not emphasized to patients by cardiologists and cardiac surgeons, because they do not want patients to be afraid of having needed surgery.
Causes of Post-CABG Cognitive Dysfunction
Most people having CABG will have at least microscopic particles of clotted blood (microthrombi) pumped into the cerebral circulation. In addition to fatty material dislodged from arterial walls and particles of clotted blood, microemboli often contain toxic material associated with surgical equipment. For example, a high prevalence of aluminum (Al) and silicon (Si) in microemboli enter the cerebral circulation, undoubtedly from surgical equipment or instrumentation. The elements Al and Si are both very toxic to the brain and anatomical damage to cerebral arteries may also be present post-surgically.
Cognitive dysfunction after CABG is likely to have multiple contributing causes, including some nonspecific effect of surgery, anesthesia, and decreased perfusion of the brain with blood (cerebral hypoperfusion), in addition to the microemboli already discussed.
Not all research agrees on the issue of whether long-term cognitive decline is actually associated with CABG. It may be that any effects associated with the surgery itself are reversible. Some research suggests that long-term cognitive decline has nothing to do with CABG, but is related to underlying or progressive disorders present in the patient such as cerebrovascular disease, prior strokes, diabetes, or hypertension.
Why Cognitive Dysfunction May Be Overlooked
MRI scans have demonstrated areas of brain damage post-CABG even in the absence of neurological abnormalities. Yet MRIs are not a standard part of post-operative evaluation.
Unless the claimant makes a specific allegation of cognitive problems, the Social Security Administration is likely to not even consider the possibility of cognitive dysfunction. However, the lack of an allegation by a claimant should not sufficient basis for disregarding the possibility of cognitive dysfunction; one cannot reasonably expect a person with impaired judgment to have an optimal ability to act in his or her own interest. The claimant’s spouse is most likely to notice personality changes and decline in thinking ability after CABG.
The Social Security Administration adjudicator should generally not rely on the cardiac surgeon’s notes to determine that the claimant has no post-operative cognitive dysfunction. Surgeons are mostly interested in surgical results involving the heart and do not perform neuropsychological tests that would be required to detect less than marked cognitive abnormalities.
After any cardiac or vascular procedure, a claimant’s representative should always consider the possibility of cognitive dysfunction. If the claimant appears normal mentally, the medical records negative, and the claimant and spouse feel there is no problem then further pursuit of this possibility probably will not be productive. However, significant numbers of cognitive dysfunction cases probably slip through the disability determination process as adjudicators concentrate only on the physical impairment.
Evaluation of Cognitive Dysfunction for Disability Purposes
Cognitive dysfunction would primarily be evaluated under the criteria for organic mental disorders, listing 12.02. Other, pre-existing mental disorders, such as personality disorders (listing 12.08) may be worsened.
Any neuropsychological testing should be done at least 3 months post-CABG, to allow clearing of any shorter term cognitive deficits.
Continue to Getting Your Doctor’s Medical Opinion About What You Can Still Do.
Go back to Winning Social Security Disability Benefits for Ischemic Heart Disease by Meeting a Listing.
